Viagra gibt es mittlerweile nicht nur als Original, sondern auch in Form von Generika. Diese enthalten denselben Wirkstoff Sildenafil. Patienten suchen deshalb nach viagra generika schweiz, um ein günstigeres Präparat zu finden. Unterschiede bestehen oft nur in Verpackung und Preis.
Jida_febmarch2008
JIDA_FebMarch2008 30/01/2008 16:12 Page 1
Volume 54 Number 1 February/March 2008
Journal of the Irish Dental AssociationIris Cumainn Déadach na hÉireann
Oral care in juvenile
JIDA_FebMarch2008 30/01/2008 16:14 Page 29
Journal of the Irish Dental Association
Oral health and orthodontic
considerations in children with juvenile
idiopathic arthritis: review of the
literature and report of a case
Abstract: Juvenile idiopathic arthritis (JIA) is a severe disease of childhood, which
comprises a diverse group of distinct clinical entities of unclear aetiology. Some
abnormality of the immune system is present in all JIA cases. In its most severe
clinical form, JIA may show localised and/or systemic complications, including
functional impairment of the affected sites. This may result in variable growth and
developmental anomalies. In many JIA cases, where the temporomandibular joint
(TMJ) is affected, mandibular growth may be restricted, thus leading to the
development of mandibular hypoplasia and/or retrognathism. As a result, it is not
uncommon for JIA patients to present with skeletal Class II and open bite
malocclusions. Furthermore, in JIA cases with unilateral TMJ involvement, craniofacial
asymmetry may occur. In such cases, early orthodontic intervention facilitates both
the skeletal and the occlusal rehabilitation.
Increased prevalence of dental caries and periodontal disease in JIA cases may be
attributed to a combination of aetiological factors, including difficulties in executing
good oral hygiene, unfavourable dietary practices and side effects from the long-term
administration of medication. In addition, an association between periodontal disease
and JIA has been reported based on their similar pattern of clinical disregulation of
the inflammatory process. This paper presents a brief description of JIA, with special
reference to dental health and orthodontic treatment considerations. In addition, a
case is presented where the appropriate orthodontic intervention led to the
establishment of a normally functioning, as well as an aesthetically pleasing,
occlusion.
KEY WORDS: juvenile idiopathic arthritis, craniofacial growth, TMJ, oral health, malocclusion,
Journal of the Irish Dental Association 2008
; 54: 29-36
Introduction to juvenile
remains unclear, although it appears to be
multifactorial, involving infectious, genetic
Philippos N Synodinos
Juvenile idiopathic arthritis (JIA) is a major
and endocrine factors.8-12
connective tissue disease and one of the
The clinical course of JIA usually involves
Athens, Greece.
most common chronic illnesses of
several sequential long or short periods of
childhood.1 Essentially, it is an early-onset
flare-ups and remissions.13-14 It may affect
form of arthritis affecting one or more joints.
any joint in the body and, in its most severe
JIA manifests before the age of 16 and
form, it may be accompanied by systemic
Athens, Greece.
remains active for more than six weeks.2 Its
complications of the cardiovascular system,
incidence is estimated at around 1-2:10,000
the urinary system and the eyes.14 Systemic
and its prevalence at 1:1,000.3-6 The
or local disturbances of growth may be
diagnostic criteria of JIA are reported in
Table
observed in JIA patients,13,14 depending on
Dublin Dental School & Hospital,
1.7 In general, three major types of JIA are
which joints are affected. This may be related
recognised: oligoarthritic; polyarthritic; and,
to either the disease or to the medication.15
systemic. These three types are briefly
Most JIA cases require chronic administration
outlined in
Table 2.2 The exact cause of JIA
of multi-drug medication, including non-
Volume 54 (1) : February/March 2008 29
JIDA_FebMarch2008 30/01/2008 16:14 Page 30
Journal of the Irish Dental Association
TABLE 1: Diagnostic criteria and types of juvenile
TABLE 2: Characteristics of the three major types of
juvenile rheumatoid arthritis.2
■ Age at onset younger than 16 years;
■ arthritis in one or more joints (defined as swelling or effusion, or
Relative frequency
the presence of two or more of the following signs: limitation of
Number of joints
range of motion; tenderness or pain on motion; and, increased
■ duration of disease >6 weeks;
■ type of onset of disease during the first six months (polyarthritic
when five or more joints are affected; oligoarthritic when less
Seropositivity –
than five joints are affected; systemic when intermittent fever is
rheumatoid factor
present and other systems of the body are involved; psoriatic;
Seropositivity –
enthesitis related; and, other), and
antinuclear antibodies
■ exclusion of other forms of juvenile arthritis.
steroidal anti-inflammatory, steroidal, disease-modifying anti-
rheumatic, and immunosuppressive drugs. The main objective of such
■ hyperdivergent facial type, increased mandibular plane angle, and
treatment is to restore and maintain quality of life for patients, while
decreased posterior facial height;21,22,33,39,40-42,44,45
alleviating pain and controlling inflammation, thereby preventing or
■ facial asymmetry in cases with unilateral TMJ involvement;20 and,
minimising joint destruction and deformity.16
■ decreased overbite, open bite or open bite
Despite treatment, an effective permanent change in the clinical
course of the disease may not be achieved until adolescence where, in
The unfavourable craniofacial growth pattern observed in many JIA
up to 70-85% of cases, a spontaneous remission is observed.17
patients is usually regarded either as primary or secondary. Primary
Additionally, prolonged administration of medication may inflict
unfavourable growth pattern is attributed to the disturbed growth of
severe side effects because of its toxicity, especially with regard to
the affected mandibular condyles,18,19,22,39,46,48,49 while secondary is
skeletal growth and development. During active phases of the disease,
attributed to the children's impaired oral function21,45 and/or
ossification at the epiphyses is accelerated, followed by premature
medication-related somatic growth retardation.20,40
closure of the epiphyseal growth plates in later stages. This may
Clinical examination may not be considered as an accurate method of
eventually result in retardation of skeletal growth and joint
diagnosing TMJ involvement in JIA patients.18,19,30,47,49,50 Therefore, the
dysfunction.2 In many JIA cases where the temporomandibular joints
application of an appropriate TMJ imaging method is often
(TMJs) are affected by the disease, growth of the mandible is
indicated.51-53 Techniques used include panoramic radiography (PR),
restricted, resulting in severe functional and aesthetic problems of the
tomography, arthrography, fluoroscopy, computerised tomography,
craniofacial complex.18-23 Complications due to the disease itself, as
magnetic resonance imaging (MRI), and radionuclide imaging.54-56
well as its treatment, may affect oral health, as evidenced by the
There is almost universal agreement that the examination of the
reported increased prevalence of caries and periodontal disease in
osseous surfaces of the TMJ is facilitated by the application of
JIA patients.24-26
tomography rather than plain film techniques.57-61 Fine bone details
can be visualised without projection limitations, while the real shape
TMJ involvement in JIA cases
and size of anatomical structures is displayed.62,63 In contrast, imaging
The reported prevalence of TMJ involvement in patients with JIA varies
of soft tissues of the TMJ is investigated in most cases by the use of
between 50% and 87%.27-34 In many such cases, temporomandibular
MRI, which is non-invasive and does not result in the patient being
joint dysfunction (TMD) is observed, presenting with restricted
exposed to ionising radiation.64,65
mandibular movements, and reduced and/or painful functional or
resting activity of the masticatory muscles. Furthermore, the
Dental health considerations in JIA patients
underlying pattern and direction of dentofacial growth may be
Although TMJ involvement in JIA is well described, only a few studies
disturbed.21,22,27,28,30,35-38 As a result, TMJ involvement in JIA patients is
report its potential adverse effects on dental health. Several factors
often associated with the development of certain craniofacial and
related to JIA may unfavourably affect oral health. TMJ-related
dental features including:
dentofacial abnormalities may be considered as contributing factors in
■ decreased mandibular length;18,19,22,39-42
the aetiology of oral diseases. TMD accompanied by impaired
■ Class II division 1 malocclusion, mostly due to mandibular
masticatory function and functional impairment of upper limbs may
30 Volume 54 (1) : February/March 2008
JIDA_FebMarch2008 30/01/2008 16:16 Page 31
Journal of the Irish Dental Association
affect toothbrushing competence.66-68 Dietary practices such as the
addressed by orthodontic/orthopaedic treatment with
consumption of softer, more sugary foods in frequent small amounts,
functional appliances.22
sweets given as consolation, the use of oral medication containing
It is not ubiquitously accepted that orthodontic treatment should be
sugar43,69-71 and factors related to psychological issues delaying
instigated early in all cases presenting malocclusions warranting
optimal dental care,26,72 all adversely affect oral health.
prompt intervention.22,84 The reluctance of many practitioners to treat
In JIA cases, an increased prevalence of dental caries24,25,73,74 and a
skeletal Class II malocclusions of JIA patients with functional appliances
higher risk for periodontal disease have been reported.75,76
while the disease remains active is due to the supported risk of flare-
Interestingly, some common clinical and pathogenic features of
up in the articular surfaces of the TMJs, resulting in a net bone loss in
periodontitis and rheumatoid arthritis have been recognised.77,78 This
the condylar growth centre.85 Whether justified or not, such delayed
implies a possible association between the two diseases that may
intervention would result in excluding any orthopaedic effect from
share a common underlying disregulation of the inflammatory
orthodontic treatment, since full remission of JIA does not occur until
response.77 Alternatively, the reported higher prevalence of
adolescence. Thus, in the majority of cases, the only choices
periodontal disease may be considered as secondary to the overall
remaining for such cases would be treating them in late adolescence,
higher plaque accumulation recorded in JIA patients,79 or to the long-
orthodontically-induced occlusal camouflaging of the underlying
term administration of medication resulting in immunosuppression,
skeletal discrepancy or, even, in extreme cases, the application of a
xerostomia, stomatitis and gingival overgrowth.80 Whatever its cause,
combination of orthodontic treatment and orthognathic
poor oral health is considered to be potentially detrimental for the
surgery.21,86,86-89 In the latter cases, costochondral grafting may be
systemic condition of JIA cases because untreated dental caries and/or
applied to serve as replacement for the completely destroyed
periodontal disease, combined with poor oral hygiene, may increase
condylar head.90,91
the risk for systemic infection, especially if the patient is taking
In contrast to postponing treatment until cessation of growth, early
immunosuppressive drugs such as methotrexate.26
treatment with functional orthodontic appliances aims to achieve and
In all JIA cases, intensive prophylactic and therapeutic measures are
maintain occlusal balance, and rehabilitate and preserve TMJ function,
required to prevent or reduce the potential damage to the dental and
while allowing for uninhibited mandibular growth.28,32,43,67 There is
periodontal tissues. Regular dental and orthodontic examination,
evidence that if functional conditions are created, growth has the
case-specific oral hygiene instructions, topical and systemic use of
potential to normalise.92 Close monitoring of the reaction of the
fluoride, appropriate dietary modification, and prescription of sugar-
condylar growth centre to functional stimuli is of utmost importance
free medicines are of prime importance for maintaining optimal
to decrease the risk of possible undesirable side effects. After the
dental health in patients with JIA.26,72 As immunosuppression is a
normalisation of craniofacial growth pattern, the application of fixed
common side effect of several anti-rheumatic drugs, it may be wise to
orthodontic appliances facilitates in finishing the orthodontically
apply antibiotic prophylaxis before dental management of certain
induced occlusal rehabilitation. In JIA cases presenting non-skeletal
JIA patients.
malocclusions, timely application of fixed orthodontic appliances only
In addition to advice on prevention, and treatment for dental diseases,
is indicated. In any JIA case warranting some kind of orthodontic
dentists should also provide information to the patient and their
treatment, it must be noted that the administered medication may
family regarding JIA's possible consequences for oral health. It is not
interfere with bone physiology, adversely affecting bone turnover,
uncommon for lay people parenting JIA patients to be totally unaware
thereby restraining orthodontic tooth movements. In all cases, light
of the effects of JIA on oral health.81
orthodontic forces should be applied to eliminate the risk of side
effects such as apical root resorption, while facilitating optimal
Orthodontic treatment considerations in JIA patients
tooth movement.23
There is extensive documentation regarding the impact that TMJ
involvement may have on the pattern of craniofacial growth in JIA
Case report
patients, resulting in the development of certain malocclusions.19-
A female patient, aged 10 years and six months, presenting
22,31,29 Accordingly, case-specific objectives of orthodontic treatment
polyarthritic JIA (involving at its onset both knees and several joints of
in JIA patients should be assessed, always keeping in mind that the
the hands), diagnosed at the age of two at the Paedo-
principal objectives in the management of the systemic disease are
Rheumatological Department of the Paediatric Clinic "Aglaia
relief of pain and discomfort, avoidance of permanent joint damage
Kyriakou" of Athens, was referred for orthodontic consultation with
and preserving an acceptable level of quality of life.23 In any JIA case,
special emphasis placed towards a comprehensive evaluation of the
the indicated orthodontic treatment can be applied on the condition
TMJ physiology. At the patient's initial admittance, the disease was in
that TMJ inflammation caused by the systemic disease is controlled by
remission using medication that included methotrexate in
proper medical care.82,83 In cases where limitation of any mandibular
combination with certain corticosteroids. Her medical history revealed
movement is observed, the application of a properly designed occlusal
a penicillin allergy. The physical examination did not show any
splint is indicated to alleviate TMD symptomatology and, while
clinically significant aberrations from normal height and weight
unloading the joints, to re-establish normal masticatory physiology.28
percentiles. Her extra-oral examination showed symmetrical
Subsequently, mandibular retrognathism/hypoplasia is typically
craniofacial features along with normal proportions of her anterior
Volume 54 (1) : February/March 2008 31

JIDA_FebMarch2008 30/01/2008 16:17 Page 32
Journal of the Irish Dental Association
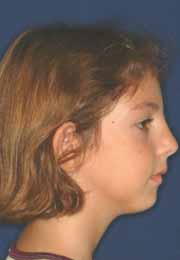
FIGURE 1: The anterior facial view of the patient at rest and smiling at
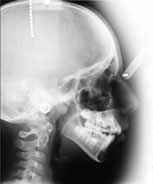
FIGURE 3: The profile view of the patient and the lateral cephalometric
her initial admittance.
radiography at her initial admittance.
FIGURE 2: The posteroanterior cephalometric radiography did not reveal
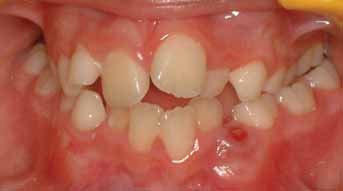
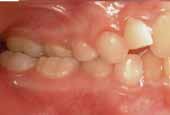
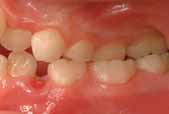
FIGURE 4: The anterior and lateral view of the patient's occlusion before
any significant asymmetry of any craniofacial structure.
the initiation of orthodontic treatment.
lower facial height (Figure 1). These were also evidenced by the
not show any signs and symptoms of TMJ dysfunction and no
evaluation of the posteroanterior cephalometric radiograph (Figure
restriction was observed in her range of movements. The examination
2). In contrast, her profile view was concave; however, at rest position
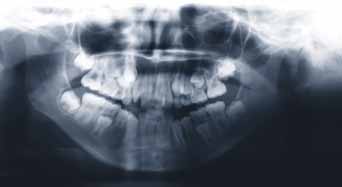
of the panoramic and the corrected sagittal tomography revealed
some interference of the lips was evident in addition to some tension
some flattening and erosive lesions on both condylar articular surfaces
of the genial muscle (Figure 3). Overall, her prominent ears affected
(Figures 5 and 6). The study of the lateral cephalometric radiograph
her facial aesthetics unfavourably and the aesthetics of her smile were
showed a hyperdivergent facial growth type presenting skeletal Class
impaired by the malaligned anterior teeth (Figure 1).
II division 1 malocclusion, mostly due to the posteriorly and
The intra-oral examination revealed a late mixed dentition stage. She
downward rotated direction of mandibular growth. An increase of the
had a Class II division 1 malocclusion with bilateral posterior crossbite,
lower to the total anterior facial height ratio was noted, in addition to
severe anterior crowding of both arches, a reduced overbite and an
a clinically significant decrease of the posterior to anterior facial height
increased overjet (Figure 4). No dental pathology was observed with
ratio. These observations implied that mandibular growth was
the exception of some plaque-induced gingival inflammation
impaired, probably as a result of the condylar growth centres having
restricted mostly to the crowded areas. The clinical TMJ evaluation did
been affected by JIA.
32 Volume 54 (1) : February/March 2008

JIDA_FebMarch2008 30/01/2008 16:17 Page 33
Journal of the Irish Dental Association
FIGURE 5: The initial panoramic radiograph of the patient.
FIGURE 8: The anterior facial view of the patient at rest and smilingafter the completion of her orthodontic treatment.
The severe dental crowding, in conjunction with the patient's
unfavourable facial growth pattern and the incompetent lips,
determined the orthodontic treatment plan, comprising the
extraction of all four first premolars. The case was assessed as one
requiring maximum anchorage, which initially involved a palatal bar
connecting the banded upper first permanent molars, followed by a
high-pull headgear. Full-mouth fixed orthodontic appliances were
sequentially applied for a total period of two years and six months. On
successive appointments, specific emphasis was placed on the
importance of the patient maintaining optimal dental hygiene. After
the completion of treatment the appliances were removed and the
FIGURE 6: The tomographical views of the patient's TMJs (corrected by
retention protocol followed. A Hawley-type retainer was used for the
the use of submental-vertex radiograph).
upper arch and a fixed lingual retainer on the lower anterior teeth.
Overall, the post orthodontic extra-oral and intra-oral clinical
examination of the patient was quite satisfactory with regard to the
occlusal and aesthetic dental and facial characteristics. No dental
pathology was observed regarding the development of either carious
(or even white spot) lesions or periodontal complications. The gingival
contour of all teeth was firm and lacking severe inflammatory signs
(no bleeding on probing, periodontal sulcus depth less than 3mm)
although some localised plaque accumulation was evident. The
occlusal view of both dental arches was normal and co-ordinated with
each other, and their midlines coincided (Figure 7). Overall, an
aesthetically pleasing smile was accomplished by the proper
alignment of the upper anterior teeth (Figure 8). The post-treatment
profile line of the patient had become almost orthognathic, although
reminiscent of its former concave form (Figure 9). Even more
important was the fact that the vertical dimension of the craniofacial
growth was controlled. The patient's lips were in contact at rest
position, although the upper lip was flatter and the nose a bit more
prominent. The post-treatment panoramic radiograph did not reveal
any clinically significant apical root resorption, interproximal dental
surfaces caries, or loss of periodontal support. The mesiodistal axial
FIGURE 7: The anterior and lateral view of the patient's occlusion after
inclination of maxillary left lateral incisor and canine did not appear
the removal of fixed orthodontic appliances.
ideal as viewed in the panoramic radiograph; however, it was
Volume 54 (1) : February/March 2008 33
JIDA_FebMarch2008 30/01/2008 16:17 Page 34
Journal of the Irish Dental Association
satisfactory on an intra-oral view. A further concern was the direction
of eruption of the lower third molars, which warranted some attention
in future recall visits (Figure 10).
The post-treatment lateral cephalometric study, although still
determining a Class II skeletal relationship, revealed a reduction of
initial values of respective variables. In addition, improved ratios of
lower anterior to total anterior facial height, and posterior to anterior
facial height, were noted. The interincisal angle was almost
normalised owing to the favourable uprighting of upper incisors and
some labial inclination of the lower incisors (Figure 11).
Finally, but most importantly, no signs or symptoms of TMJ
dysfunction were recorded throughout orthodontic treatment.
1. Sullivan, D.B., Cassidy, J.T., Petty, R.E. Pathogenic implications of age and
onset in JRA. Arthritis Rheum 1975; 18: 251-255.
FIGURE 9: The profile view of the patient and the lateral cephalometric
2. Cassidy, J.T. Juvenile rheumatoid arthritis. In: Kelley, W.N., Harris, E.D.,
radiography after the completion of her orthodontic treatment.
Ruddy, S., Sledge, C.B., (eds.). Textbook of Clinical Rheumatology, Vol 2,
5th ed., WB Saunders Co, Philadelphia, 1997: 1207-1224.
3. Towner, S.R., Michet, C.J. Jr., O'Fallon, W.M., Nelson, A.M. The
epidemiology in juvenile arthritis in Rochester, Minnesota. Arthritis Rheum
1983; 26: 1208-1213.
4. Kunnamo, I., Kallio, P., Pelkonen, P. Incidence of arthritis in urban Finnish
children. Arthritis Rheum 1986; 29: 1232-1238.
5. Anderson Gäre, B. Juvenile Chronic Arthritis. A Population Based Study in
Epidemiology, Natural History and Outcome (thesis). University of
Göteborg, Göteborg, Sweden 1994.
6. Symmons, P., Jones, M., Osborne, J., Sills, J., Southwood, T.R., Woo, P.
Paediatric rheumatology in the UK: data from the British Paediatric
FIGURE 10: The final panoramic radiograph of the patient.
Rheumatology Group National Diagnostic Register. Br J Rheumatol 1996;
23: 1975-1980.
7. Petty, R.E., Southwood, T.R., Baum, J., Bheattay, E., Glass, D.N.,
Manners, P. et al. Revision of the proposed classification criteria for juvenile
idiopathic arthritis. J Rheumatol 1998; 25: 1991-1994.
8. Petty, R.E., Tingle, E.J. Arthritis and viral infection. J Pediatr 1988; 113:
9. Lang, B.A., Shore, A. A review of current concepts on the pathogenesis of
JRA. J Rheumatol 1990; 17 (Suppl. 21): 1-15.
10. Harris, E.D. Jr. Rheumatoid arthritis: pathophysiology and implication for
therapy. N Engl J Med 1990; 322: 1277-1289.
11. Nepom, B. The immunogenetics of JRA. Rheum Dis Clin North Am 1991; 17:
12. Madson, K.L., Moore, T.L., Lawrence, J.M. III, Osborn, T.G. Cytokine
levels in serum and synovial fluid of patients with JRA. J Rheumatol 1994; 21:
13. Schaller, J.G. Chronic arthritis in children. Juvenile rheumatoid arthritis. Clin
Orthop 1984; 182: 79-89.
14. Davidson, J. Juvenile idiopathic arthritis. Eur J Radiol 2000; 33: 128-134.
15. Calabro, J.J., Holgersson, W.B., Sonpal, G.M., Khoury, M.L. JRA: a general
review and report of 100 patients observed for 15 years. Semin Arthr
Rheumatol 1976; 5: 257-298.
FIGURE 11: The juxtaposition of the tracings of the lateral
16. Schiff, M. Emerging treatments for rheumatoid arthritis. Am J Med 1997;
cephalometric radiographs taken before (white line) and after (navyblue line) the completion of the orthodontic treatment.
102 (Suppl.): 11S-15S.
34 Volume 54 (1) : February/March 2008
JIDA_FebMarch2008 30/01/2008 16:17 Page 35
Journal of the Irish Dental Association
17. Ansell, B.M., Bywaters, E.G.L. Alternate day corticosteroid therapy in
37. Hanna, V.E., Rider, S.F., Moore, T.L., Wilson, V.K., Osborn, T.G.,
juvenile chronic polyarthritis. J Rheumatol 1974; 1: 176-186.
Rotskoff, K.S., et al. Effect of systemic onset JRA on facial morphology and
18. Larheim, T.A., Haanaes, H.R. Micrognathia, TMJ changes and dental
TMJ form and function. J Rheumatol 1996; 23: 155-158.
occlusion in JRA of adolescents and adults. Scand J Dent Res 1981; 89: 329-
38. Mericle, P.M., Wilson, V.K., Moore, T.L., Hanna, V.E., Osborn, T.G.,
Rotskoff, K.S., et al. Effect of polyarticular and pauciarticular onset JRA on
19. Larheim, T.A., Haanaes, H.R., Ruud, A.F. Mandibular growth TMJ changes
facial and mandibular growth. J Rheumatol 1996; 23: 159-165.
and dental occlusion in JRA. Scand J Rheumatol 1981; 10: 225-233.
39. Bache, C. Mandibular growth and dental occlusion in JRA. Acta Rheumatol
20. Stabrun, A., Larheim, T.A., Höyeraal, H.M., Rösler. Reduced mandibular
Scand 1964; 10; 142-153.
dimensions and asymmetry in JRA. Pathogenetic factors. Arthritis Rheum
40. Barriga, B., Lewis, T.M., Law, D.B. An investigation of the dental occlusion
1988; 31: 602-611.
in children with juvenile chronic arthritis. Angle Orthod 1974; 44: 329-335.
21. Kreiborg, S., Bakke, M., Kirkeby, S., Michler, L., Vedtofte, P., Seidler, B.,
41. Stabrun, A.E. Impaired mandibular growth and micrognathic development
et al. Facial growth and oral function in a case of JRA during an 8-year
in children with JRA. A longitudinal study of lateral cephalographs. Eur J
period. Eur J Orthod 1990; 12: 119-134.
Orthod 1991; 13: 423-434.
22. Kjellberg, H., Fasth, A., Kiliaridis, S., Wennenberg, B., Thilander, B.
42. Rönning, O., Barnes, S.A.R., Pearson, M.H., Pledger, D.H. Juvenile
Craniofacial structure in children with juvenile chronic arthritis compared
chronic arthritis: a cephalometric analysis of the facial skeleton. Eur J Orthod
with healthy children with ideal or postnormal occlusion. Am J Orthod
1994; 16: 53-62.
Dentofacial Orthop 1995; 107: 67-78.
43. Walton, A.G., Welbury, R.R., Foster, H.E., Thomason, J.M. Juvenile
23. Pedersen, T.K. Clinical aspects of orthodontic treatment for children with
chronic arthritis: a dental review. Oral Dis 1999; 5: 68-75.
juvenile chronic arthritis. Acta Odontol Scand 1998; 56: 366-368.
44. Twilt, M., Schulten, A.J., Nicolaas, P., Dulger, A., van Suijlekom-Smit,
24. Storhaug, K. Dental health problems in juvenile chronic arthritis. EULAR Bull
L.W. Facioskeletal changes in children with juvenile idiopathic arthritis. Ann
1977; 3: 88-92.
Rheum Dis 2006; 65: 823-825.
25. Siamopoulou, A., Mavridis, A.K., Vasakos, S., Benecos, P., Tzioufas,
45. Larheim, T.A. Comparison between three radiographic techniques for
A.G., Andronopoulos, A.P. Sialochemistry in juvenile chronic arthritis. Br J
examination of the TMJ in JRA. Acta Radiol Diagn 1981; 22: 195-201.
Rheumatol 1989; 28: 383-385.
46. Rönning, O., Väliaho, M-L., Laksonen, A-L. The involvement of the TMJ in
26. Welbury, R.R., Thomason, J.M., Fitzgerald, J.L., Steen, I.N.,
JRA. Scand J Rheumatol 1974; 3: 89-96.
Marshall, N.J., Foster, H.E. Increased prevalence of dental caries and
47. Karhulahti, T., Rönning, O., Jämsa, T. Mandibular condyle lesions, jaw
poor oral hygiene in juvenile idiopathic arthritis. Rheumatology 2003;
movements, and occlusal status in 15-year-old children with JRA. Scand J
42: 1445-1451.
Dent Res 1989; 98: 17-26.
27. Larheim, T.A., Höyeraal, H.M., Stabrun, A.E., Haanaes, H.R. The TMJ in
48. Engel, M.B., Richmond, J., Brodie, A.G. Mandibular growth disturbances
JRA. Scand J Rheumatol 1982; 11: 5-12.
in rheumatoid arthritis of childhood. Am J Dis Child 1949; 78: 728-743.
28. Grosfeld, O. The orthodontist in the team – treatment for children with
49. Forsberg, M., Agerberg, G., Persson, M. Mandibular dysfunction in
rheumatoid arthritis. Eur J Orthod 1989; 11: 120-124.
patients with juvenile chronic arthritis. J Cranio Dis 1988; 2: 201-208.
29. Karhulahti, T., Rönning, O., Jämsa, T. Mandibular condyle lesions, jaw
50. Rönning, O., Väliaho, M-L. Involvement of the facial skeleton in JRA. Ann
movements and occlusal status in 15-year-old children with JRA. Scand J
Radiol 1975; 18: 347-353.
Dent Res 1990; 53: 17-26.
51. Christiansen, E.L., Thompson, J.R. Temporomandibular Joint Imaging.
30. Olson, L., Eckerdal, O., Hallonsten, A-L., Helkimo, M., Koch, G.,
Mosby Year Book, St Louis, 1990; 39-128, 147-164.
Anderson Gäre, B. Craniomandibular function in juvenile chronic arthritis.
52. Resnick, D., Yu, J.S., Sartoris, D. Imaging. In: Kelley, W.N., Harris, E.D.,
Swed Dent J 1991; 15: 71-83.
Ruddy, S., Sledge, C.B., (eds.). Textbook of Clinical Rheumatology, Vol 2,
31. Ronchelez, M.V., Hilario, M.O., Goldenberg, J., Lederman, H.M., Faltin,
5th ed., WB Saunders Co, Philadelphia, 1997; 626-686, 1207-1224.
K. Jr, de Azevedo, M.F., et al. TMJ and mandibular growth alterations in
53. Cohen, P.A., Job-Deslandre, C.H., Lalande, G., Adamsbaum, C. Overview
patients with JRA. J Rheumatol 1995; 22: 1956-1961.
of juvenile idiopathic arthritis (JIA). Eur J Radiol 2000; 33: 94-101.
32. Pearson, M.H., Rönning, O. Lesions of the mandibular condyle in juvenile
54. Goaz, P.W., White, S.C. Temporomandibular Joint. In: Goaz, P.W., White,
chronic arthritis. Br J Orthod 1996; 23: 49-56.
S.C., (eds.). Oral Radiology: Principles and Interpretation. CV Mosby Co, St
33. Sidiropoulou-Chatzigianni, S., Papadopoulos, M.A., Kolokithas, G.
Louis 1987: 560-600.
Dentoskeletal morphology in children with juvenile idiopathic arthritis
55. Friedland, B. Clinical radiological issues in orthodontic practice. Semin
compared with healthy children. J Orthod 2001; 28: 53-58.
Orthod 1998; 4: 64-78.
34. Twilt, M., Mobers, S.M., Arends, L.R., ten Cate, R., van Suijlekom-Smit,
56. Quintero, J.C., Trosien, A., Hatcher, D., Kapila, S. Craniofacial imaging in
L. J Rheumatol 2004; 31: 1418-1422.
orthodontics: historical perspective, current status, and future
35. Kjellberg, H. Craniofacial growth in juvenile chronic arthritis. Acta Odontol
development. Angle Orthod 1999; 69: 491-506.
Scand 1998; 58: 360-365.
57. Omnell, K.A., Petersson, A. Radiography of the TMJ utilising oblique lateral
36. Wenneberg, B., Kjellberg, H., Kiliaridis, S. Bite force and
transcranial projections: comparison of information obtained with
temporomandibular disorder in children with juvenile chronic arthritis. J
standardised technique and individualised technique. Odont Revy 1976; 27:
Oral Rehab 1995; 22: 633–641.
Volume 54 (1) : February/March 2008 35
JIDA_FebMarch2008 30/01/2008 16:17 Page 36
Journal of the Irish Dental Association
58. Goldman, S.M., Taylor, R. Radiographic examination of the abnormal
77. Mercado, F.B., Marshall, R.I., Klestov, A.C., Bartold, P.M. Relationship
temporomandibular joint. J Prosth Dent 1983; 49: 711-714.
between rheumatoid arthritis and periodontitis. J Periodontol 2001; 72: 779-
59. Habets, L.M.H., Bezuur, J.N., Jimenez Lopez, V., Hansson, T.L. The OPG:
an aid in TMJ diagnostics. III. A comparison between lateral tomography
78. Havemose-Poulsen, A., Westergaard, J., Stoltze, K., Skjodt, H.,
and dental panoramic radiography (Orthopantomography). J Oral Rehab
Danneskiold-Samsoe, B., Locht, H. et al. Periodontal and haematological
1986; 16: 401-406.
characteristics associated with aggressive periodontitis, juvenile idiopathic
60. Larheim, T.A., Johannessen, S., Tveito, L. Abnormalities of the
arthritis, and rheumatoid arthritis. J Periodontol 2006; 77: 280-288.
temporomandibular joint in adults with rheumatic diseases: a comparison
79. Reichert, S., Machulla, H.K., Fuchs, C., John, V., Schaller, H.G., Stein, J.
of panoramic, transcranial, transpharyngeal radiography with tomography.
Is there a relationship between juvenile idiopathic arthritis and
Dentomaxillofac Radiol 1988; 17: 109-113.
periodontitis? J Clin Periodontol 2006; 33: 317-323.
61. Petersson, A., Rohlin, M. Rheumatoid arthritis of the TMJ: evaluation of
80. Lehmann, T., Day, R.O., Brooks, P.M. Toxicity of antirheumatic drugs.
three different radiographic techniques by assessment of observer
Med J Aust 1997; 166: 378-383.
performance. Dentomaxillofac Radiol 1988; 17: 115-120.
81. Tanchyk, A. Treating growth and TMJ abnormalities in JRA. J Am Dent Assoc
62. Wilson, C., Williamson, E. Use of a submental vertex analysis for producing
1994; 125: 1617-1621.
quality TMJ radiographs. Am J Orthod 1976; 70: 200-207.
82. Wennenberg, B., Kopp, S., Grondahl, H.G. Long-term effect of
63. Williams, B. Oriented lateral temporomandibular joint laminographs. Angle
intraarticular injections of a glucocorticosteroid into the TMJ. A clinical and
Orthod 1983; 53: 228-233.
radiographic 8-year follow up. J Craniomandib Disord Facial Oral Pain 1991;
64. Anderson, Q.N. The current role of magnetic resonance imaging in
temporomandibular joint treatment planning. In: Stegenga, B., deBont,
83. Alstergren, P., Appelgren, A., Appelgren, B., Kopp, S., Lundeberg, T.,
L.G.M., (eds.). Management of Temporomandibular Joint Degenerative
Theodorsson, E. The effect on joint fluid concentration of neuropeptide Y
Diseases. Birkhäuser Verlag, Basel, Switzerland 1996: 87-97.
by intra-articular injection of glucocorticoidin in patients with
65. Murakami, K.I., Segami, N. Current role of diagnostic arthroscopy in
temporomandibular joint arthritis. Acta Odontol Scand 1996; 54: 1-7.
temporomandibular joint treatment planning. In: Stegenga, B., de Bont,
84. Kitai, N., Kreiborg, S., Bakke, M., Paulsen, H.U., Moller, E., Darvann,
L.G.M., (eds.). Management of Temporomandibular Joint Degenerative
T.A. et al. Three-dimensional magnetic resonance image of the mandible
Diseases. Birkhäuser Verlag, Basel, Switzerland 1996: 99-110.
and masticatory muscles in a case of juvenile chronic arthritis treated with
66. Tanchyk, A.P. Dental considerations for the patient with juvenile
the Herbst appliance. Angle Orthod 2002; 72: 81-87.
rheumatoid arthritis. Gen Dent 1991; 39: 330-332.
85. Proffit, W.R. Treatment planning: the search for wisdom. In: Proffit, W.R.,
67. Jämsa, T., Rönning, O. The facial skeleton in children affected by
White, R.P. Jr, eds. Surgical Orthodontic Treatment. St Louis, Mosby Year
rheumatoid arthritis – a roentgen–cephalometric study. Eur J Orthod 1985;
Book, 1991: 158-159.
86. Turpin, D.L., West, R.A. Juvenile rheumatoid arthritis: a case report of
68. Burden, D., Mullaly, B., Sandler, J. Orthodontic treatment of patients with
surgical/orthodontic treatment. Am J Orthod 1978; 73: 312-320.
medical disorders. Eur J Orthod 2001; 23: 363-372.
87. Oye, F., Bjornland, T., Store, G. Mandibular osteotomies in patients with
69. Roberts, I.F., Roberts, G.J. Dental disease in chronically sick children. J Dent
juvenile rheumatoid arthritis disease. Scand J Rheumatol 2003; 32: 168-173.
Child 1981; 48: 346-351.
88. Leshem, D., Thompson, B., Britto, J.A., Forrest, C.R., Philips, J.H.
70. Hobson, P. Sugar-based medicines and dental disease. Comm Dent Health
Orthognathic surgery in juvenile rheumatoid arthritis. Plast Reconstr Surg
1985; 2: 57-62.
2006; 117: 1941-1946.
71. Shaw, L., Glenwright, H.D. The role of medications in dental caries
89. Singer, S.L., Southall, P.J., Rosenberg, I., Gillet, D., Walters, M.
formation: need for sugar-free medications for children (review).
Mandibular distraction osteogenesis and maxillary osteotomy in a Class II
Paediatrician 1989; 16: 153-155.
division 1 patient with chronic juvenile arthritis. Angle Orthod 2006; 76:
72. Walton, A.G., Welbury, R.R., Thomason, J.M., Foster, H.E. Oral health
and juvenile idiopathic arthritis: a review. Rheumatology 2000; 39: 550-555.
90. Mayro, R.F., De Lozier, J.B.D., Whitaker, L.A. Facial reconstruction
73. Drecka-Kuzan, K. Comparative survey on the incidence of dental caries in
consideration in rheumatic diseases. Rheum Dis Clin North Am 1991; 17:
children with rheumatoid fever and rheumatoid arthritis. Rheumatologia
1971; 9: 125-133.
91. Svensson, B., Feldman, G., Rindler, A. Early surgical-orthodontic
74. Zifer, S.A., Sams, D.R., Potter, B.J. Clinical and radiographical evaluation
treatment of mandibular hypoplasia in juvenile chronic arthritis. J
of juvenile rheumatoid arthritis: report of a case. Special Care Dent 1994; 14:
Craniomaxillofac Surg 1993; 21: 67-75.
92. Pedersen, T.K., Gronhoj, J., Melsen, B., Herlin, T. Condylar condition and
75. Gleissner, C., Willershausen, B., Kaesser, U., Bolten, W.W. The role of risk
mandibular growth during early functional treatment of children with
factors for periodontal disease in patients with rheumatoid arthritis. Eur J
juvenile chronic arthritis. Eur J Orthod 1995; 17: 385-394.
Med Res 1998; 3: 387-392.
76. Miranda, L.A., Fischer, R.G., Sztajnbok, F.R., Figueredo, C.M.,
Gustafsson, A. Periodontal conditions in patients with juvenile idiopathic
arthritis. J Clin Periodontol 2003; 30: 969-974.
36 Volume 54 (1) : February/March 2008
Source: http://smilesareus.gr/page57.php
www.aidsmap.comissue 158 july 2006 why GPs need to be integrated into HIV-positive care page 4 primary care at HIV clinics is your clinic providing GP services? page 14 immunisation guidelines new vaccination guidance for HIV-positive people page 8 does efavirenz cause depression? a new study suggests otherwise page 3 anti-HIV therapy adds thirteen years to post-AIDS survival page 13
New clinical trial investigates APOKYN for treating debilitating morning akinesia in Park. Page 1 of 4 May 13, 2013 11:09 AM Eastern Daylight Time New clinical trial investigates APOKYN for treating debilitating morning akinesia in Parkinson's disease patients LOUISVILLE, Ky.--(BUSINESS WIRE)--US WorldMeds today announced the launch of a new clinical trial investigating APOKYN® (apomorphine hydrochloride injection) as a rapid and reliable treatment for "morning akinesia" in Parkinson's disease. AM IMPAKT, short for Apokyn for Motor IMProvement of Morning AKinesia Trial, is a Phase IV, multi-center, open-label study that will enroll approximately 100 subjects at 12 study sites across the US.











